Dr Manish Singhal - The best Cancer Specialist in Delhi
Prostate Cancer Specialist in Noida, Delhi NCR
Prostate Cancer
Prostate cancer, also known as carcinoma of the prostate, is the development of cancer in the prostate, a gland in the male reproductive system. Most prostate cancers are slow growing; however, some grow relatively fast.
Prostate cancer might be slow-growing sometimes, but that doesn't make prostate cancer patients any less vulnerable to Covid-19. So what can be done? Dr. Manish Singhal, a renowned Oncologist in India and the best Prostate Cancer doctor in Noida, along with his team of expert healthcare professionals, is offering at-home cancer treatment, telemedicine services, video call consultations, and more to prostate cancer patients maintaining all the necessary preventive measures.
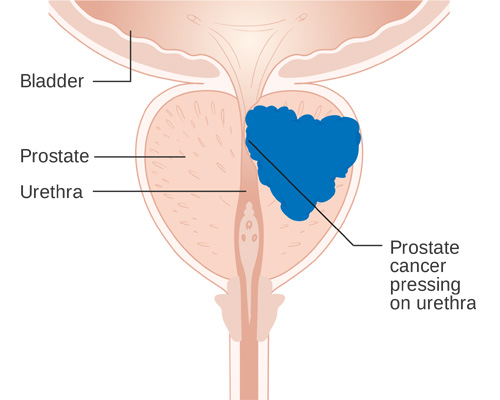
The cancer cells may spread from the prostate to other parts of the body, particularly the bones and lymph nodes. it may initially cause no symptoms. In later stages it can cause difficulty urinating, blood in the urine, or pain in the pelvis, back or when urinating.
A disease known as benign prostatic hyperplasia may produce similar symptoms. Other later symptoms may include feeling tired due to low levels of red blood cells
Types of Prostate Cancer
There are a few types of prostate cancer and the condition is often present in different parts of the prostate. The precursor to prostate cancer is known as prostatic intraepithelial neoplasia, and is also found in different locations within the prostate.
This is a benign (non-cancerous) type of tumor of the prostate. The prostate grows larger and squeezes the urethra. This prevents the normal flow of urine. BPH is a very common problem. For some men the symptoms may be severe enough to need treatment or surgery.
This type of tumor is the most frequent form of prostate cancer and accounts for 90 to 95% of prostate cancer. Prostatic adenocarcinoma is occurring in the cells lining the glandular organ of the prostate, the area responsible for the secretion of the chemicals that make up a large portion of seminal fluid. The most common site of origin of prostate cancer is the peripheral zone where two thirds of the prostate glandular tissue is located. Typically, prostatic adenocarcinoma is a slow growing form of cancer, and when found early there is a good chance of achieving cures.
This type of cancer is made of small round cells. It is a very aggressive form of prostate cancer that does not lead to a change in prostate specific antigen (PSA). It thus can be more difficult to detect than adenocarcinoma. The small cell carcinoma has usually reached an advanced form upon detection.
This type of prostate cancer is non glandular and like small cell carcinoma does not lead to an increase in prostate specific antigens (PSA). Squamous cell carcinoma is a very aggressive form of cancer.
ough all of the layers of the muscle into the connective tissue outside the stomach but has not grown into the peritoneal lining or serosa. It has not spread to any lymph nodes or surrounding organs (T3, N0, M0).
This type of cancer is extremely rare and account for less than 0.1% of primary prostate cancer. Prostatic sarcoma occurs in relatively younger men between the ages of 35 and 60. The tumor is made up of prostate cancer cell types that are capable of developing into connective tissues, lymphatic vessels, and blood vessels originating from smooth muscles of the prostate.
Twenty-five percent of cases present with metastatic disease at the time of diagnosis. Prostatic sarcoma remains localized for a viable period of time before it spreads locally to the bladder, rectum or perineum. Over more time the tumor will spread to distant locations like the lungs, brain, bones or liver. The most common sites of distant metastasis are the lungs.
This type of cancer rarely develops in the prostate but derives from primary tumors present in the bladder or urethra.
Stages of Prostate Cancer
There are two types of staging of prostate cancer:
- The clinical stage is based on the results of tests done before surgery, which includes DRE, biopsy, x-rays, CT and/or MRI scans, and bone scans. X-rays, bone scans, CT scans, and MRI scans may not always be needed. They are recommended based on the level of serum PSA; the size of the cancer, which includes its grade and volume; and the clinical stage of the cancer.
- The pathologic stage is based on information found during surgery, plus the laboratory results, referred to as pathology, of the prostate tissue removed during surgery. The surgery often includes the removal of the entire prostate and some lymph nodes.
Prevention of Prostate Cancer
Tumor Board Evaluation
According to the expert Oncologist in Delhi, treatment approaches for prostate cancer range from prostate removal surgery, called a prostatectomy, to non-surgical treatments such as radiation, Brachytherapy and hormone therapy. The choice of prostate cancer treatment depends on factors such as how fast the cancer is growing, how much it has spread, the age and overall health. Men whose cancer is detected while confined to the prostate gland have an excellent chance for successful treatment with minimal or short-term side effects.
Oncologist in Noida Dr. Manish Kumar Singhal see several thousand men who have prostate cancer each year. That experience helps them to guide patients toward the most appropriate treatment approach. We take great care to ensure patients understand the benefits and risks associated with each treatment option.
Surgery
Surgery is the mainstay of prostate cancer treatment. As a single treatment method – meaning that no radiation, chemotherapy or additional treatment is anticipated – surgery is an effective way to treat cancer confined to the prostate gland.
Our Surgical Oncologists use great care and proven techniques to remove the prostate (radical prostatectomy) while making every effort to spare the muscles and nerve bundles that control urination and sexual function.
External Beam Radiation Therapy
Radiation therapy uses high-powered beams or other radiation to kill cancer cells. Cancer cells are generally more sensitive to the harmful effects of radiation compared to normal tissues. Radiation may be used to treat most stages of prostate cancer, with or without surgery, depending on each patient’s overall health and cancer severity.
Dr. Manish Kumar Singhal oncologists have developed a method that uses special imaging devices to precisely track the internal movement of the prostate while daily radiation beam treatments are administered. Intensity modulated radiation therapy (IMRT) uses gold markers implanted in the prostate to allow radiologists to precisely guide radiation beams to their intended target, reducing radiation exposure to the rectum and bladder. IMRT safely delivers more radiation to the prostate while sparing surrounding tissue, resulting in increased cure rates.
Radiation after Surgery
Radiation therapy is also commonly used after surgery to treat the prostate bed (the area formerly containing the prostate). Pathologists examine the removed prostate under a microscope to determine whether any cancer cells, possibly may not have been completely removed via surgery. If suspected traces of cancer are thought to remain, additional radiation therapy may be administered at some point following surgery.
Post-surgical radiation treatments reduce the chances of recurrence. Treatment usually begins within two to three months following surgery and lasts for six to seven weeks. Radiation therapy may also be administered if the PSA level rises after surgery. At all times, the patient is considered to be a member of the treatment team and is involved in decision making.
Brachytherapy Radiation
Brachytherapy involves the implantation of rice-sized radioactive seeds into the prostate to destroy the cancer. In Permanent Prostate Brachytherapy, implanted seeds are left in place, but their radioactivity decreases over time.
Hormone Therapy
When advanced prostate cancer can’t be treated through surgery or other means, hormone therapy is an option. Hormone therapy reduces the supply of male sex hormones that make prostate cancers grow faster. In most cases, hormone therapy is not a cure, but may help control prostate cancer. This can be done by surgery (Removal of both testis) or injection Goserelin to be taken life long.
Expectant Management
Expectant Management may be an option for men over 70, those in poor health, or men whose cancer is small and slow growing. (Expectant management was formerly referred to as watchful waiting.)



